Cell-based immunotherapy — CAR-T cell therapy — has revolutionized the treatment of several cancers. The therapy uses genetically engineered T cells to target and attack certain types of leukemia and lymphoma. While it can eliminate cancer in some patients who would otherwise die from it, it also comes with a risk of a host of side effects, some of which can affect brain function and can even be life-threatening.
In a performance study, researchers from Washington University School of Medicine in St. Louis found that a simple blood test performed before CAR-T cell therapy began could determine which patients were in the days and weeks after CAR-T cell therapy. prone to neurotoxic side effects. When they analyzed blood samples from patients before, during and after CAR-T cell therapy, they found that levels of a protein called neurofilament light chain (NfL) were higher in patients with neurotoxic complications . High levels of NfL were present even before treatment began, and its levels remained high throughout treatment and for a month after treatment. The results of the study were published online in the journal JAMA Oncology on September 1, 2022, with the title “Assessment of Pretreatment and Posttreatment Evolution of Neurofilament Light Chain Levels in Patients Who Develop Immune Effector Cell–Associated Neurotoxicity Syndrome”.
The new research may help physicians predict these life-threatening side effects and enable them to start administering neurotoxicity-reducing therapy early in patients receiving CAR-T cell therapy. It also opens the door to developing ways to prevent or reduce the risk of these side effects before CAR-T cell therapy begins.
“Our study shows that some patients treated with CAR-T cells had previously undetected neuronal damage at baseline,” said senior author Omar H. Butt, MD, of Washington University School of Medicine in St. Louis. This was before preparing them for this treatment. We don’t know the origin of this damage, but it appears to predispose them to neurotoxic complications. If we understand who is at risk for these complications, we can take early steps to prevent It may reduce its severity.”
As a general marker of neuronal damage, NfL protein has been used to measure or monitor the severity of several neurological diseases, including Alzheimer’s disease and multiple sclerosis.
“Measurements of NfL in blood are used as a way to assess the effectiveness of potential new treatments for multiple sclerosis,” said study co-author Beau M. Ances, MD, professor of neurology at Washington University School of Medicine in St. Louis. “We plan to continue our research, Find the root cause of neuronal damage in these cancer patients. This is a unique collaboration possible at the University of Washington because we have some of the top experts in CAR-T cell therapy and leading experts in neurodegenerative diseases. It provides It’s a great opportunity to bridge the gap and bring these areas together to try to solve a troubling problem and help patients.”
The new study was relatively small, involving 30 patients treated at Washington University St. Louis School of Medicine Sterman Cancer Center and Case Western Reserve University Case Comprehensive Cancer Center.
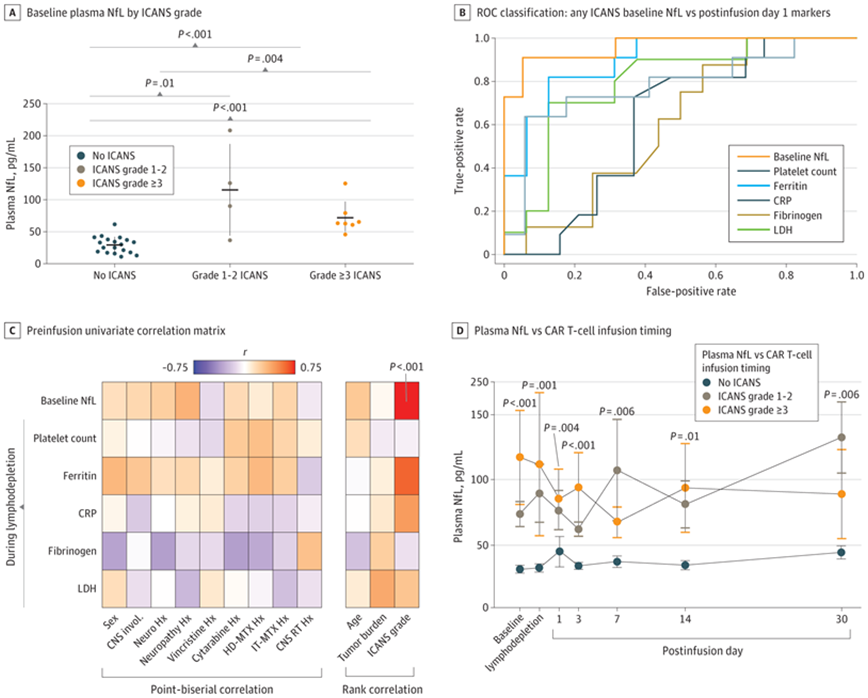
Baseline levels of NfL distinguish patients who do not experience neurotoxic side effects from those who experience any degree of such side effects. The authors plan to continue analyzing data from more patients to see if a larger sample size allows them to identify patients at risk for mild, moderate or severe complications.
These complications vary from person to person and can include anything from difficulty concentrating, memory problems, confusion, difficulty reading and headaches to seizures, strokes and brain swelling. Doctors mainly deal with these complications by giving high doses of steroids and sometimes immunomodulatory therapy to try to reduce inflammation. Knowing who is at risk for the most dangerous side effects is very helpful, since these methods unfortunately weaken the cancer-fighting effects of CAR-T cells, and doctors want to avoid them as much as possible.
Another mystery is that the rise in NfL levels was pre-existing and remained largely stable even as some patients recovered from neurotoxic side effects. This suggests that NfL levels indicate something is wrong, but do not reflect what caused the patient’s complications.
“We’re only seeing the tip of the iceberg of the actual disease process, and that’s where a lot of our future research is going,” Butt said. “We’re trying to better understand what’s causing these changes. At a later stage, even after the symptoms have resolved, we’re still See an increase in NfL levels.”
Co-author Dr. Armin Ghobadi of Washington University School of Medicine in St. Louis added, “We are conducting a study at Sterman Cancer Center to see if these patients continue to have subtle symptoms in terms of cognitive changes or long-standing deficits. “